During the following four weeks (Feb 19-March 12 2017) Trisha Phippard, a doctoral researcher at the Institute for Anthropological Research in Africa (IARA) at KU Leuven University (Belgium), will be sharing some reflective notes about her field research in and around Kikwit. This doctoral project is embedded in a larger research project dealing with technology cultures in the DR Congo.
Post #2. A new sort of epidemic at Kikwit’s hospital
The Hôpital Général de Référence Kikwit I – the principal hospital Kikwit – is currently experiencing an epidemic. However, unlike the severe Ebola outbreak that unfortunately made the town internationally famous in 1995, this time it is not a virus that is replicating rapidly and spreading through the hospital grounds. No, the hospital is now facing an epidemic of a very different nature: an epidemic of doctors.
I am being rather provocative by referring to the rapid proliferation and oversupply of medical personnel as an epidemic, but this is a very real public health problem here, and the ramifications are troubling. For a hospital of 286 beds, the ideal number of doctors serving the institution is at most 7 (according to the hospital’s Médecin Directeur). Yet, in Kikwit’s main state health facility, the number is hovering around 70, ten times the required amount. This doesn’t include the almost 400 nurses, the 15 administrative managers, and the numerous other support personnel.

Kikwit’s primary hospital. 13.02.2015 © Trisha Phippard
This abundance of doctors perhaps counters the development narrative of countries like Congo needing more doctors and medical expertise, but the reality here is that the medical practitioners now outnumber the patients dramatically. The hospital clearly doesn’t need any more doctors, but the government keeps sending them, as a mass of young physicians is churned out of medical school every year. However, this is not just an outcome of the number of students that are pursuing medicine, attracted by the perceived respect and comfortable lifestyle afforded to doctors. The crux of the problem is the highly distributed nature of the health system in Congo and the many rural health districts. Most of these young doctors refuse a remote posting in the ‘bush’, if they can, instead finding political influence through an uncle or friend in Bandundu to secure their posting to an urban area like Kikwit, where they can live a more comfortable and social life.
The extent of this political interference in response to the appeal of urban centres is revealed more clearly when you contrast the situation in Kikwit with that at the reference hospital in Mosango, located 115km along the road to Kinshasa. Although still a part of the state health infrastructure, Mosango’s hospital is governed (in all aspects, including staffing decisions) by the Catholic diocese rather than directly by the state. For approximately the same number of beds as in Kikwit, they have just 4 physicians and 66 other paramedical personnel. In other more rural health districts in the province, reference hospitals often have just 1 or 2 doctors.
This draw towards urban institutions like Kikwit’s hospital also represents a missed opportunity for these young practitioners, because a physician in a remote health zone is granted much more responsibility and practical experience. The Médecin Chef de Staff at the reference hospital in Pay Kongila, a rural health district based 100km from Kikwit, estimates that he has gained about five years’ experience in the less than two years of work as a self-described ‘bush doctor’. As a young man with no family to worry about, the living conditions in the village are no problem, and he sees the value in this post for his career advancement. He tells me that here the work is not divided amongst many hands, and there are no specialists to consult; he has to “do it all.”

Doing ‘pansement’ (cleaning wounds and changing bandages) in the nearly empty female surgical ward. 04.07.2016 © Trisha Phippard
In Kikwit, by contrast, this rapidly growing number of doctors have very little to do, cultivating an air of boredom and discontent. Hospital staff go about their days perfunctorily, both redundant and underpaid. In my time here, I have found that it is not uncommon to witness Kafkaesque scenes like I observed last week, when working in the surgical ward I followed a group of 6 doctors doing rounds in a room with only 3 occupied beds (not to mention the 4 nurses and 2 interns changing bandages or doing menial tasks in the ward, nor the several other nurses hanging out in the office).
I am at the hospital laboratory today. We wait until after 10 for the first patient to arrive. At the radiology department where I also spend a lot of time, it is the same story. Mornings are usually spent sitting around in boredom, waiting for either the electricity to come on or the patients to arrive.

The products of a full day’s work at the radiology department – 7 cases in total, a relatively high turnout. 05.05.2016 © Trisha Phippard
But the patients don’t come, at least not in the volume needed to make the hospital thrive. Now, in the height of the dry season, the sporadic flow of patients has slowed even more, to barely a trickle. This is in part because parents often prefer to pay school fees at the end of the year before coming to have a medical problem looked at. But the doctors tell me it is also a matter of competition. Kikwit is now has a number of polycliniques – smaller, private, and often better equipped than the slumbering old state institutions like the general hospital. A consultation at the hospital is expensive (especially when diagnostic procedures like laboratory tests, x-rays, or ultrasounds are required) and patients know that they may be met with unreliable technologies, counterfeit medicine, and other small supplementary charges from the doctors themselves. Many choose instead to seek out alternatives, biomedical or otherwise.
This ‘epidemic’ thus has a real economic impact, for both doctors and patients. The state keeps sending doctors, but the hospital has no money to pay them the local premium that should supplement the state salary to make it a livable wage. So doctors find their own ways to make money on the side, with either the hospital or the patients suffering as a result. An explicitly forbidden – but still popular – route is the pharmasac: a bag of medicines that the doctor sells privately, undermining the hospital pharmacy (which is traditionally a main source of hospital income). This means that the hospital has even less money in its operating budget to pay staff or buy essentials like soap, which many of the wards often experience shortages of. Other doctors have resorted to using fake applications on their smartphones to perform extra “tests” (like glucose levels), and technicians and nurses demanding money for “gloves” which they don’t use. Patients have no choice, so they pay up.
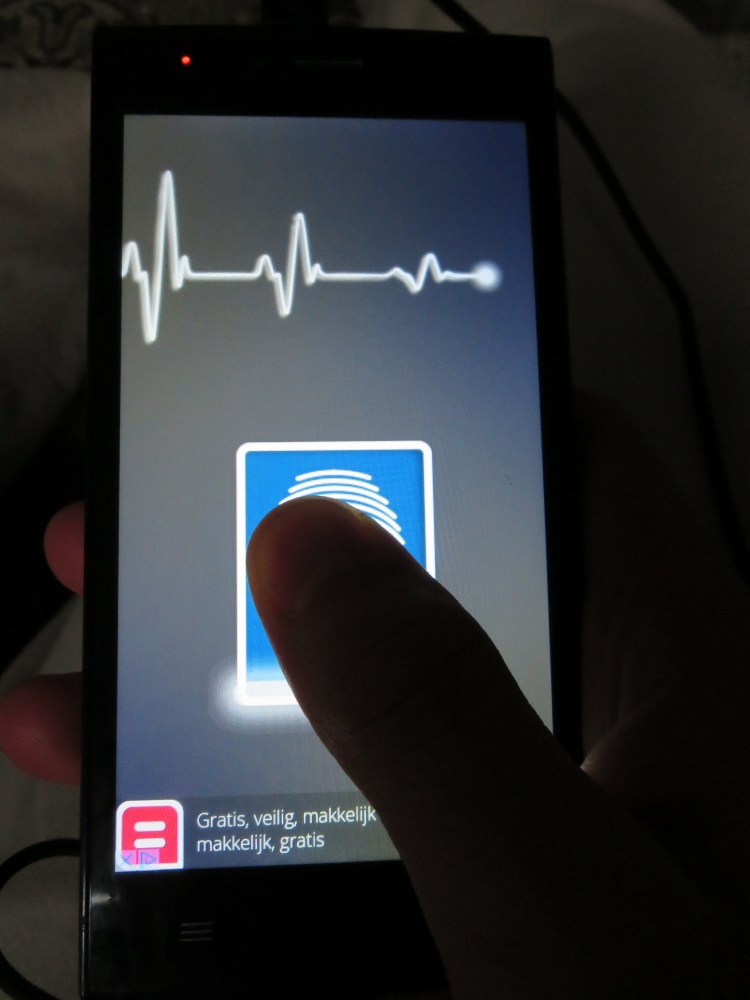
An example of the type of fraudulent smartphone app used by doctors to earn extra income (downloaded on my husband’s phone as an example only). 28.09.2016 © Trisha Phippard
It is a situation without an easy solution. The hospital, its patients, and the doctors themselves all suffer from their growing numbers. There is simply neither the workload nor the resources to sustain them, but many still resist transfer to more remote districts in need. Like with many aspects of the vitality of various state hospitals in this region, it often comes down to the efforts of the individual Médecin Directeur of each hospital to try to make the institution thrive – or at least survive. It falls on these doctors to try to find external financial support and material donations, and in this case to inspire cooperation and allegiance amongst the staff (and discipline those who choose to undermine the institution or patient security). This is a daily struggle, and it seems unjust that it often depends on the character and the contacts of the individual doctor leading the hospital as to whether it will have the necessary materials and resources to serve its population. But in the absence of a more robust state health system, it is a struggle that will no doubt continue.
Discussion
No comments yet.