During the following four weeks (Feb 19-March 12 2017) Trisha Phippard, a doctoral researcher at the Institute for Anthropological Research in Africa (IARA) at KU Leuven University (Belgium), will be sharing some reflective notes about her field research in and around Kikwit. This doctoral project is embedded in a larger research project dealing with technology cultures in the DR Congo.
Post #4. Pay Kongila’s ‘moto ambulance’: Part Two
We are rushing to secure the patient on the moto ambulance before the storm arrives in Kulungu-Siki. Although the moto is outfitted with a chest strap to secure the patient, it’s not a perfect system. For unconscious or semi-conscious patients like we have today, it is necessary to tie down the arms and legs with additional straps to prevent them from flopping about (a danger to the driver) and to help keep the patient upright on the moto. Someone fetches a mosquito net, which Saddam cuts into strips to secure her limbs for the bumpy road ahead. It is difficult to secure the chest strap, with her head lolling and unconscious weight flopping her around like a rag doll.

Loading the patient onto the moto ambulance in Kulungu-Siki. 14.11.2016 © Trisha Phippard
The thunder is growing more and more threatening, so as soon as she is secured we start the tough trip back to Pay Kongila, driving as fast as we possibly can. The dark clouds chase us ominously, with rain sputtering on and off as we outrun the storm. The sand is treacherous, especially at this speed, and the dramatic tension is palpable, the urgency of the case amplified by the urgency of the weather. We have to stop a few times to re-fasten the straps when her limbs come flying out of the restraints and onto Saddam’s shoulders, nearly toppling the moto, and to give her water as she slips in and out of consciousness. It is a struggle to make sure she is comfortable, but also firmly tied down. At one point she urinates all over Saddam, soiling his clothes because he doesn’t have protective clothing. He takes it in stride, saying this sometimes happens with blood.

Re-fastening the restraints on the route back to Pay Kongila. 14.11.2016 © Trisha Phippard
When we arrive at the hospital, we take her straight to the Salle D’Urgence, where the hospital staff take over and we go off to rest. Less than 45 minutes later, the Médecin Chef de Staff calls me to come to the Bloc Opératoire immediately and change into surgical scrubs and cap in a hurry. The woman’s case is urgent; we need to operate right away. There is no time for diagnostic tests or a ‘wait and see’ period of observation. Later, the doctor tells me that in the West, they would have performed emergency ultrasound exams and other diagnostic procedures before arriving at that decision, but the result – to open her up – would surely have been the same.
We tie up our surgical masks and head into the operating room, trailed by a number of young interns. An anesthesiologist and a young assistant are already busy draping the patient and laying out all the surgical tools. They have turned on the generator so they can use the more powerful AC-powered lamps rather than the feeble solar lights that illuminate the hospital. The surgeons are wearing big black gumboots and long plastic aprons to the floor, a precaution I immediately understand when the small portable suction machine refuses to work and a volcano of blood erupts when they make the incision. The case is a ruptured ectopic pregnancy, and her abdomen is completely filled with blood. It is a long, slow, methodical procedure to repair the rupture, soak up all the blood (one absorbent pad at a time), and suture each layer back together.
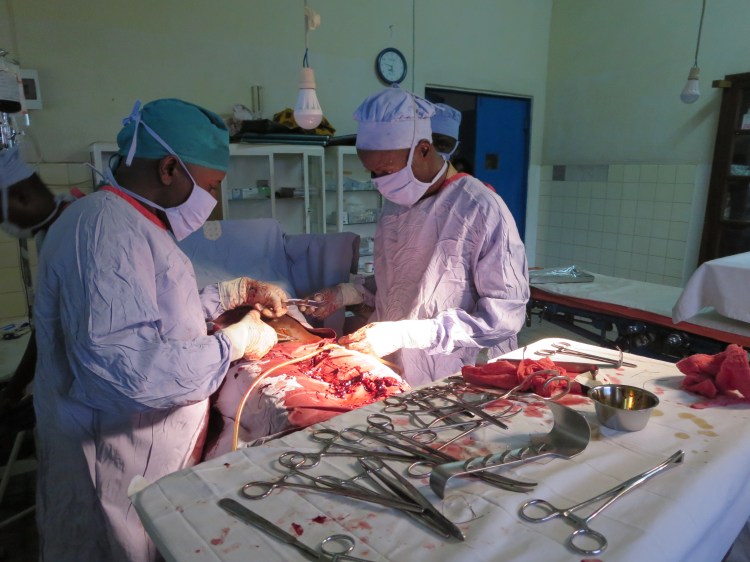
Mid-surgery in the operating room in Pay Kongila. 14.11.2016 © Trisha Phippard
It is hot in here, and my back aches from standing in one position. The doctor and assistant both have sweat pouring off them; I wonder where they find the strength to perform these difficult surgeries day after day. After 75 minutes, they are finally closing her up and preparing to take her back to the ward for close observation and further blood transfusions. The surgeon says that she would have certainly died today if she had been left in the village.
This was surely a life saved, thanks to the moto ambulance program. It’s a good day. But this episode also speaks to the precarity of biomedical intervention in this region, the fragility of the health structures in place. If Memisa’s moto ambulance program hadn’t granted a moto to this health zone, the patient surely would have died. If someone hadn’t been here to pay the $6 in fuel for the trip after the community fund ran dry, she certainly wouldn’t have made it. If Saddam had been out on another call, it would have been too late.

The surgical facilities the patient would have encountered if left at the village health centre in Kulungu-Siki. 14.11.2016 © Trisha Phippard
The community is quite pleased with the concept of the moto, and many, many lives have been saved in the 10 months since it has been introduced in this district. The president of the community committee organizing the moto, a tradipraticien himself, tells me that there is much desire to use it. But the financing is limited. Patients aren’t asked for a single franc congolais to use the service, so the maintenance and purchasing of the fuel depends on the redistribution of part of the consultation fees collected at all zone’s health centres. However, many people can’t afford to pay these fees, so revenue is limited. Even when there is enough money in the envelope to buy the fuel to fetch a patient, sometimes these patients can’t afford the required diagnostic exams or treatment procedures when they arrive at the hospital.
Later in the evening, a formal presentation is made of a second moto ambulance for the Pay Kongila health zone. Everyone seems happy to have it, and the potential to extend the reach of patient evacuations is clear. What is less clear is how the community will find the money to finance it in order to make the most of this new technology to save lives and reduce the negative health outcomes for those living in rural and isolated areas.
Discussion
No comments yet.